A Note From CODE: We are pleased to welcome Paul Bruning, Executive Director of Orthopedics, and a member of AAOE. Read Paul’s other articles, The Real Value of Patient-Reported Outcomes, and What it Will Take to Reach Transparency in Health Care.
As we continue to speed toward value-based care, the questions executives are trying to figure out are:
1. How they will measure value
2. How their organizations will be paid based on value.
The widely accepted formula for measuring value is outcomes/cost – with the gold standard of outcomes being patient-reported outcomes (PROs). In my experience, once executives understand what PROs measure and some simple real-life applications, they agree PROs will play an important role in helping them define value.

Value varies based on your perspective
Value varies depending on the person. An example I love to use is the value of a hamburger. A fast food hamburger, even though it’s not known for its quality, may be highly valuable to some based on its low cost. A gourmet hamburger, known more for its fresh and unique ingredients, may be more valuable to some based on the quality. Both hamburgers are considered highly valuable depending on who you ask. Measuring value in health care is really no different. Value to a patient, payer, provider, or executive is all quality/cost. While this may seem overly simplistic, these two components can be very complex.
Measuring value by understanding the patients’ perception of their care
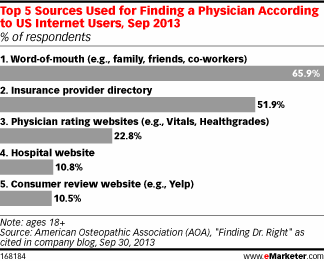
Savvy executives often prioritize quality ahead of cost. There have been numerous articles, like this one that documents the impact quality and patient experience (patient’s perception) have on revenue. Even this study from Advisory Board estimates a 10% increase in loyalty (loyalty is driven by perception) could generate more than $22 million in revenue for the average hospital. Further, with word of mouth driving 60%+ of referrals (perception is key here too), I think we can agree it makes sense for executives to prioritize high quality.
One way executives can gain insights into the patient’s perception of their care, in real time, is by implementing a patient-reported outcomes program. This is because PROs measure exactly what patients value: improvement in pain, function, and quality of life. These surveys are taken prior to intervention (at first visit) and then at specified time frames during and following treatment. When PROs indicate average or better than average improvement, it’s a good indicator that patients will have a positive perception of their care.
PROs give insight into the health of your organization
Beyond using PROs to measure patients’ perception of their care, PROMs are very sophisticated tools that can be used to evaluate, compare, and benchmark within an organization, across geographic areas, and across provider taxonomies.
Providers showing higher patient improvement scores can be used to help train others on their methods. Simply asking patients if they felt their wait time was acceptable or if the pre-op class was helpful can give executives valuable insight into opportunities to positively influence a patient experience.
These examples above are just the tip of the iceberg. Often, executives incorporate PROs into their dashboards. PRO data, cost of care, overhead figures, and process outcome measures provide direct evidence of the value of care your organization provides. This can be reported back to providers, team members, and other service lines of a larger health system. The dashboard can provide advanced warning if there is a decrease in quality, perception of that quality, or value of care.
Patient-Reported Outcomes can be a powerful negotiation tool
In case increasing referrals, improving, quality, and patient experience is not enough, PRO data can be taken to payers and used as a negotiation tool. As an executive, if you have the ability to have PROs, process data, and cost data on hand and analysis done, you can be on equal footing with the payer. Payers know the total cost of care for each provider. However, they do not know patient outcomes. Comparing the total cost of care, PROs, and patient experience can demonstrate unique value opportunities that could benefit both the payer and the health care organization. Those providers who have demonstrated value based on quality and cost should have better levels of reimbursement. This is true value-based reimbursement. PROs are at the center of this analysis of value.
PROs role in public and private APMs
BPCI-Advanced, CJR, and Centers of Excellence (Holy Cross Orthopedics is a COE for GE and Bridge Health) do reward organizations for evaluating and monitoring PROs. These metrics play an important role in reimbursement. As these programs move into maturity, PROs will play a larger role in demonstrating value.
Further, while PRO data is not largely made public in today’s market, as patients become more aware of and impacted by costs, they will start to evaluate the value of the care they seek. Organizations currently collecting, and ready to share patient-reported outcomes data, will have an advantage over those organizations that are forced to become late adopters. Executives within health care understand this and are starting to move towards a routine collection of PROs, because they know if you aren’t measuring now, they will be.
Schedule A Call With a PRO Expert!
Need more help with your PRO related questions? CODE can help! Schedule a call with a CODE expert today to get you on your way to better harnessing your patient reported outcomes.





